Placental Problems | Placenta 101
The placenta is the organ responsible for nourishing the baby and ensuring successful pregnancy progression. Its major functions are to supply oxygen and nutrients to the baby and remove waste products.
The mother’s blood and the baby’s blood come into very close contact in the placenta.
The placenta is attached to the mother through the wall of the uterus and to the baby via the umbilical cord.
Essential Information
- The placenta is formed in the uterus during pregnancy, creating a vital connection between the developing baby and the mother.
- Soon after conception, the placenta implants in the wall of the uterus with the umbilical cord connecting the baby to the placenta.
- The placenta is a flat, oval organ and is the place where maternal and fetal blood are brought into very close contact – yet they do not mix – so that the mother can supply oxygen and nutrients to the baby and at the same time remove waste products from the baby’s blood.
- Once the baby is born, these waste products are removed by the lungs (carbon dioxide) and kidneys (urea and creatinine).
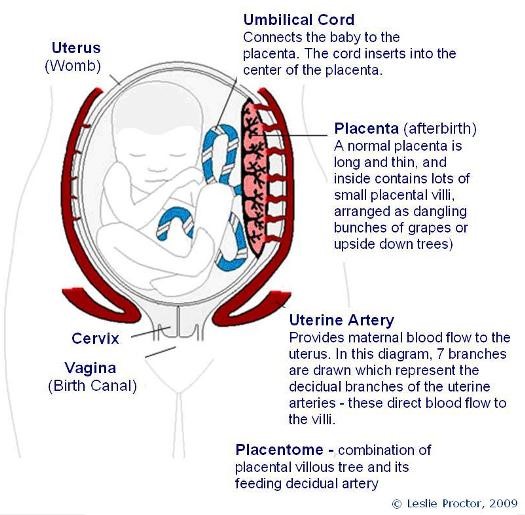
Overview
The placenta is connected to the baby by the umbilical cord and to the mother through her inner uterine wall. The umbilical cord contains three blood vessels: two arteries and one vein. Through the umbilical arteries, the fetus pumps “used” blood with waste and carbon dioxide into the placenta, while blood that is rich in nutrients and oxygen returns from the placenta back to the baby via the larger umbilical vein. The normal placenta is wide and thin, and inside contains lots of small placental villi, arranged as many dangling bunches of grapes to allow the exchange between mother and fetus.
The mother sends blood to the placenta via her uterine arteries – these become much wider (dilated) in pregnancy to deliver more maternal blood to nourish the developing fetus. In the non-pregnant state, only 50mL/minute of maternal blood enters the uterus. By mid-pregnancy, this has increased 5-fold to 250mL/minute and on, up to over 700mL/minute at the end of pregnancy. The mother achieves this by increasing her circulating blood volume (from 5L to 6-7L) and cardiac output.
Conditions of the Placenta
There is a variety of clinical conditions in pregnancy that are associated with the placenta. These include fetal growth restriction/placental insufficiency, preeclampsia, placenta praevia, vasa praevia, placenta accreta spectrum (PAS) disorders, placental chorioangiomas and amniotic band syndrome/sequence.
Care and research
The Frances Bloomberg Centre for Women’s and Infants’ Health at Mount Sinai Hospital in Toronto has a specialized Placenta Clinic that is dedicated to caring for women whose pregnancies are at risk for, or complicated by, placental diseases. Specialists provide the best clinical care possible, while raising the importance of “placentology” in teaching medical students, residents, clinical fellows, health care workers and international visitors. That is how knowledge in the field continues to advance.
We also have a wide-ranging research program. Our studies encompass clinical research and translational/basic research projects, all designed to advance our understanding and the future prevention of ill health attributed to the placenta.
Genetic research and the placenta
The human placenta shares about 95% of its genetic code with small rodents, such as mice. This is important because it is now possible to manipulate the genetic code in mice and breed them (transgenic mice) to see which genes are critical for mammalian placental development. The Lunenfeld-Tanenbaum Research Institute at Mount Sinai Hospital is a world leader in advancing our understanding of both human and mouse placental development.
Whilst many individual aspects of placental function (such as nutrient transport, oxygen transfer, blood flow regulation) can be studied in the laboratory, only a few components can be measured “risk-free” or non-invasively in a real-time clinical setting.
